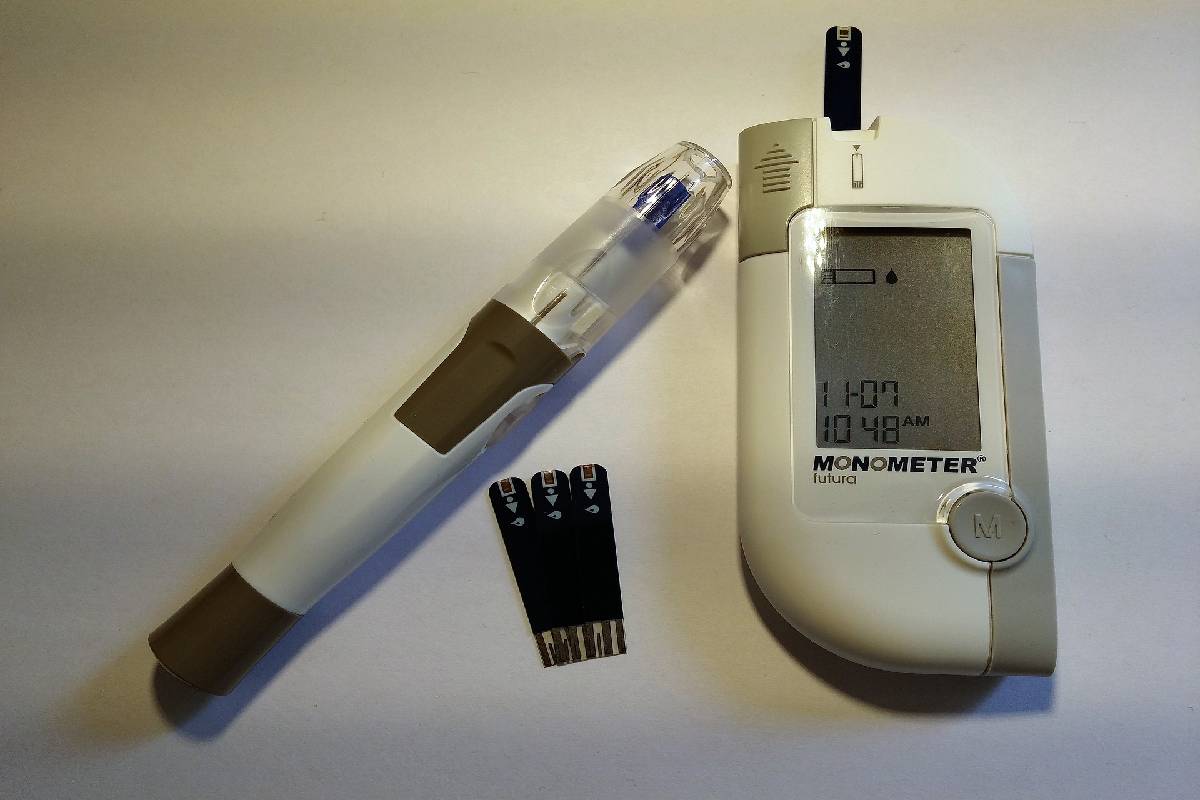
Hyperglycemia is the medical term for abnormally high blood sugar (glycemia). Blood sugar levels stand measured by a blood sample taken from a vein or a small cold-blooded piece. It can remain measured in a laboratory in isolation or other blood tests or measured using a portable glucometer. This small device allows frequent monitoring of blood glucose levels without needing a doctor’s office or laboratory.
Hyperglycemia is a typical sign of diabetes (type 1 diabetes and type 2 diabetes) and pre-diabetes. Normal ranges for blood glucose measurements may vary slightly among different laboratories. Still, in general, fasting glucose levels (early morning before breakfast) stay considered normal if it is between 70 and 100 mg/dL. Glucose levels may increase slightly above this range after a meal. Random blood glucose measurements are usually less than 125 mg/dL.
Blood hyperglycemia occurs when your body fails to transport sugar from the blood to the cells effectively.
Table of Contents
When uncontrolled, it can lead to diabetes.
A 2012 study reported that 12-14% of American adults had type 2 diabetes, while 37-38% stood classified as pre-diabetic.
It means that half of all American adults suffer from diabetes or pre-diabetes.
Sometimes, however, hyperglycemia is not the result of diabetes. Other conditions or situations that can lead to hyperglycemia, including:
- Pancreatitis (inflammation of the pancreas)
- Pancreatic cancer
- Hyperthyroidism (hyperactive thyroid gland)
- Cushing syndrome (high level of blood cortisol)
- Hormone-secreting tumours, including glucagonoma, pheochromocytoma or growth hormone-secreting tumours
- Severe trauma to the body, such as heart attack, stroke, various trauma or serious illnesses, can temporarily lead to hyperglycemia
- Taking certain medications, including prednisone, estrogens, beta-blockers, glucagon, oral contraceptives, phenothiazines and others, may increase blood sugar levels
Sometimes it can also be just a matter of food hygiene and life. That is what we will deal with in this article.
Here are 15 simple ways to decrease your glycemic levels naturally:
Also read: Ten Healthy Delicious and Easy-to-Make Dinners
1. Play sports regularly
Regular physical activity can help you lose weight and increase your insulin sensitivity.
Increased insulin sensitivity means that your cells can make better use of the sugar available in the bloodstream.
The exercises also help your muscles use blood sugar to produce energy for muscle contraction.
If you have trouble monitoring your blood sugar, you should check your blood levels regularly. It will help you learn how your body reacts to different activities and keep your blood sugar neither too high nor too low.
There are suitable forms of exercise that include dumbbells, brisk walking, running, biking, dancing, hiking, swimming and more.
Conclusion: Exercise increases insulin sensitivity and helps your muscles consume sugars in the blood. It
2. Control your carbohydrate intake
Your body turns carbohydrates into sugars (essentially glucose), then insulin integrates sugars into cells.
When you consume too many carbohydrates or have problems with your insulin, this process fails, and blood glucose levels increase.
However, there are several ways to address this.
The American Diabetes Association (ADA) recommends controlling carbohydrate intake by counting carbohydrates or using a food exchange system.
Some studies have shown that these methods can also help you plan your meals properly, improving your blood glucose resistor.
Many lessons also show that a low-carb diet assistances reduce blood sugar levels and prevent blood sugar spikes.
Better yet, a low-carb diet can help control blood sugar levels in the long run.
You can learn more in this article about healthy low-carb diets in diabetics.
Conclusion: Carbohydrates stand broken down into glucose, which increases blood sugar levels. Reducing carbohydrate intake can help control blood sugar.
3. Increase your fibre intake
Fibre slows down the digestion of carbohydrates and the absorption of sugar. Thus, they promote a more gradual increase in blood sugar.
In addition, the type of fibre plays an important role.
There are two types of fibre: insoluble and soluble fibre. Although both are important, soluble fibre is particularly capable of lowering blood sugar levels.
What’s more, a high-fibre diet can help manage type 1 diabetes by improving blood glucose control and reducing blood sugar drops.
Foods that are tall in fibre include vegetables, fruits, legumes and whole grains.
The suggested daily intake of fibre is about 25 grams for women and 38 grams for men. That’s about 14 grams per 1000 calories.
Conclusion: Eating many fibres can help control blood sugar; soluble dietary fibres are the most effective.
4. Drink water and stay hydrated
Drinking enough water can help you keep your blood sugar within normal limits.
In addition to avoiding dehydration, it helps your kidneys eliminate excess blood sugar in the urine.
An observational study showed that those who drank more water had a lower risk of developing hyperglycemia.
Drinking water regularly rehydrates your blood, lowers your sugar levels and reduces the risk of diabetes.
Keep in mind that other non-calorie water drinks are the best alternatives. Sugar-sweetened beverages increase blood sugar, increase weight and increase the risk of diabetes.
Conclusion: Staying hydrated can reduce your blood sugar levels and help you prevent diabetes. Water is the best choice.
5. Control your portions
Portion control helps regulate caloric intake and can lead to weight loss.
Therefore, controlling your weight promotes normal blood sugar levels and has been shown to reduce the risk of developing type 2 diabetes.
Monitoring your portions also helps to reduce caloric intake and therefore peaks in hyperglycemia.
Here are some helpful tips for controlling your portions:
- Measure and weigh your portions.
- Use smaller plates.
- Avoid restaurants as much as you can.
- Read food labels and check portion sizes.
- Keep a food diary.
- Eat slowly.
Conclusion: The more you control what you eat, the better the control you will have over your blood sugar.
6. Choose diets with a low glycemic index
The glycemic directory stayed developed to assess the variation in your glycemic response following the ingestion of carbohydrate-containing foods.
The amount and type of carbohydrates both determine how a food affects blood sugar levels.
Eating foods with low glycemic indexes has been shown to reduce long-term blood sugar levels in type 1 and type 2 diabetics.
Even though the glycemic index of diets is essential, the amount of carbohydrates you ingest also counts.
Foods with a low glycemic catalogue include seafood, meat, eggs, oats, barley, beans, lentils, legumes, sweet potatoes, corn, yam, most non-starchy fruits and vegetables.
Conclusion: It is crucial to choose foods with a low glycemic index and monitor your overall carbohydrate intake.
7. Control your stress level
Stress can affect your blood sugar.
Hormones such as glucagon and hydrocortisone stay secreted during stress. These hormones cause an increase in blood sugar levels.
One study has shown that sports, relaxation and meditation significantly reduce stress and reduce blood sugar in students.
Sport and relaxation methods such as yoga and stress-reduction based on mindfulness can also correct insulin secretion problems in chronic diabetes.
Conclusion: Controlling stress levels through sports or relaxation methods such as yoga will help you control blood sugar levels.
8. Monitor your blood sugar levels
“Anything that can remain measured can be achieved.”
Measuring and nursing blood glucose levels can also help you control them.
For example, tracking helps you determine if you need to make adjustments in your meals or medications.
It can also help you discover how your body reacts to certain foods.
Try to measure your blood glucose daily, and write down these levels in a journal.
Conclusion: Monitoring your blood sugar and keeping a diary will help you adjust foods and medications to achieve optimal sugar levels.
9. Get enough and quality hours of sleep
Poor sleep patterns and a lack of rest also affect your blood sugar levels and insulin sensitivity. They can upsurge appetite and promote weight gain.
Sleep deprivation cuts the release of growth hormones and increases cortisol levels. Both play an essential role in the control of blood sugar.
What’s more, good sleep is about both quantity and quality. It is best to get enough high quality sleep every night.
Conclusion: Good sleep helps maintain blood glucose control and promotes a healthy weight. Poor sleep can disrupt critical metabolic hormones.
10. Eat foods rich in chromium and magnesium
High sugar levels and diabetes remain also linked to micronutrient deficiencies.
Examples include deficiencies in chromium and magnesium minerals.
Chromium is involved in the metabolism of carbohydrates and lipids. It also helps to control blood sugar levels, and a lack of chromium can predispose you to carbohydrate intolerance.
However, the mechanisms behind it are not fully known. Studies also report mixed results.
Two studies of patients with diabetes have shown that chromium has benefits for long-term blood glucose control. However, another study showed no benefit.
Foods high in chromium include egg yolks, whole grain products, bran-rich cereals, coffee, nuts, green beans, broccoli and meat.
Magnesium has also remained shown to affect your blood sugar levels, and a magnesium deficiency has remained linked to a higher risk of developing diabetes.
In one study, a society with the highest magnesium intake had a 47% lower risk of developing diabetes. However, if you already consume many foods high in magnesium, you probably will not be able to benefit from the supplements.
Foods rich in magnesium include dark leafy green vegetables, whole grains, fish, dark chocolate, bananas, avocados, and beans.
Bottom Line: Eating foods high in chromium and magnesium regularly can help prevent deficiencies and reduce blood sugar problems.
Also read: Six types of foods You must-have on a Balanced Menu